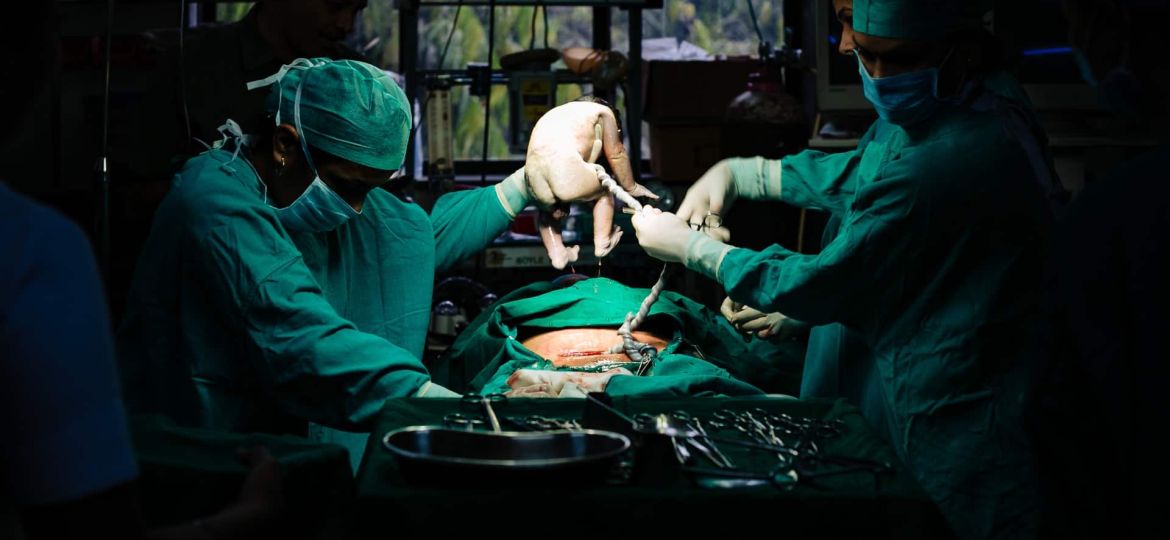
In France, about 1 in 5 deliveries is by cesarean section, not by vaginal delivery. This operation can be planned in advance, and is called a scheduled cesarean section, or it can be performed in an emergency, before or during labor. It is quite quick and usually lasts about an hour – most of this time being spent suturing the incision. The type of anesthesia used and the possibility for the father to stay with the mother depend on the conditions under which the cesarean section is performed. However, scheduled and emergency cesarean sections also have many similarities. How are they performed? Why are they decided? Let’s take a look.
How is a cesarean section performed?
The hospitalization can take place the same morning or the day before the operation. In any case, the mother-to-be must be fasting. Beforehand, she will have removed all jewelry and nail polish and taken an antiseptic shower. After the reception, the questions and the usual medical checks, the mother will put on the outfit planned for the operation and will be taken to the operating room. A urinary catheter and an infusion will be put in place.
Most of the time, the anesthesia is local. In the case of scheduled cesarean sections, it is often a spinal anesthesia. In the case of emergency cesarean sections, if an epidural is already in progress, it is then extended for the necessary time. General anesthesia is reserved for extreme emergencies (or in case of contraindications).
The incision made, just above the pubis – previously shaved – is called a hysterotomy. It is 10 to 15 cm long and crosses the abdominal and uterine walls. In the vast majority of cases, it is performed horizontally. Once the baby is removed from the womb, skin-to-skin contact is immediately offered or not, depending on the circumstances. The incision is stitched or stapled, the first care is given to the newborn and the mother is monitored in the recovery room for about 2 hours.
What are the reasons for a cesarean section?
There are many reasons why the medical team may decide to perform a cesarean section. When the operation is scheduled, the cause may be a multiple pregnancy, especially in the case of triplets. The cause can be a maternal health reason, such as: pre-eclampsia, a heart problem that makes pushing risky, a placenta that is too low (placenta previa) that creates a risk of hemorrhage, a virus such as HIV or an outbreak of genital herpes that can contaminate the baby, etc. Stunted growth of the child or macrosomia (estimated birth weight greater than 4.5 kg) are also factors in the option of a scheduled operation.
During labor, excessive or prolonged fetal distress, detected by the presence of abnormalities in the heartbeat of the unborn child, is a frequent cause of emergency cesarean section. Other common reasons for emergency cesarean sections include failed forceps extraction, failure of cervical dilation despite medication, severe maternal bleeding, preeclampsia, or very premature birth.
What are the after-effects and risks?
Like any operation, a cesarean section involves risks. In addition to the possibility of a reaction to the anesthesia, the most frequent complication is a urinary tract infection due to the catheter. Much more rarely, a cesarean section can cause a misplacement of the placenta in a subsequent pregnancy, phlebitis, infection of the uterus, etc.
As for the postpartum period, discharge from the maternity hospital is later than for vaginal delivery: it usually takes place between 4 and 7 days after the birth. Moreover, the mother must be extremely careful not to carry more weight than her baby, even more than a mother who gave birth by vaginal delivery. As for the scar, it remains quite discreet and is generally not visible, even in a bathing suit.

